Table of Contents - Can You Get Herpes From a Hot Tub? 5 Real Risks Exposed
This blog post may contain affiliate links. As an Amazon Associate I earn from qualifying purchases.
Article Meta: Medically Reviewed by , [MD/DO/RN, Specialty] | Last Updated: June 2026
⚠️ Medical Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you have symptoms, a potential exposure, or health concerns, consult a licensed healthcare provider. Always follow the guidance of your physician or qualified health professional regarding any medical condition.
No — you cannot get herpes from a hot tub. The herpes simplex virus (HSV) is one of the most common infections worldwide, and it’s entirely natural to wonder what “casual contact” really means when you’re sharing warm water with strangers or friends.
Most answers online stop at “no.” But if you’ve developed a mysterious rash after a soak, or you’re unsure what’s safe when a partner has herpes, a one-word answer isn’t enough. You deserve the science behind it.
This guide explains exactly why water transmission is biologically impossible, what the one genuine hot tub health risk actually looks like, and how herpes does spread — through surfaces, shared items, and direct contact — so you can stop worrying about the wrong things.
If you are wondering, “can you get herpes from a hot tub?” the answer is no—chlorine and bromine inactivate HSV almost on contact. Use The Transmission Hierarchy to evaluate any risk: water (zero) → surfaces (negligible) → shared saliva items (low) → direct skin contact (actual risk).
- Hot tubs & pools: Zero HSV transmission risk — halogen disinfectants destroy the virus
- Toilet seats & surfaces: Near-zero risk — HSV dies quickly on dry, cold surfaces (Mayo Clinic)
- Real spa risk: Hot tub rash is bacterial (Pseudomonas), often mistaken for herpes
- Kissing & sharing items: Genuine HSV-1 risk — direct oral contact and saliva do transmit (CDC)
Can You Get Herpes From a Hot Tub?
When asking, can you get herpes from a hot tub, the definitive answer is no; you cannot get it from a hot tub, a pool, or a shared bath. The herpes simplex virus is inactivated almost immediately in properly maintained hot tub water, according to the Public Health Agency of Canada. Sharing a hot tub with someone who has herpes carries no meaningful risk of water-based transmission — the chemistry and biology work decisively against the virus.
To understand why, it helps to think about HSV transmission risk as a hierarchy. The Transmission Hierarchy places water at the absolute bottom — zero risk — dry surfaces near-zero, and direct skin-to-skin mucosal contact at the top, where actual transmission occurs. This mental model clarifies every anxious question in this article. Hot tubs, pools, and bath water all sit at the same level: the bottom.
As the chart below illustrates, environment plays a decisive role in HSV survival.
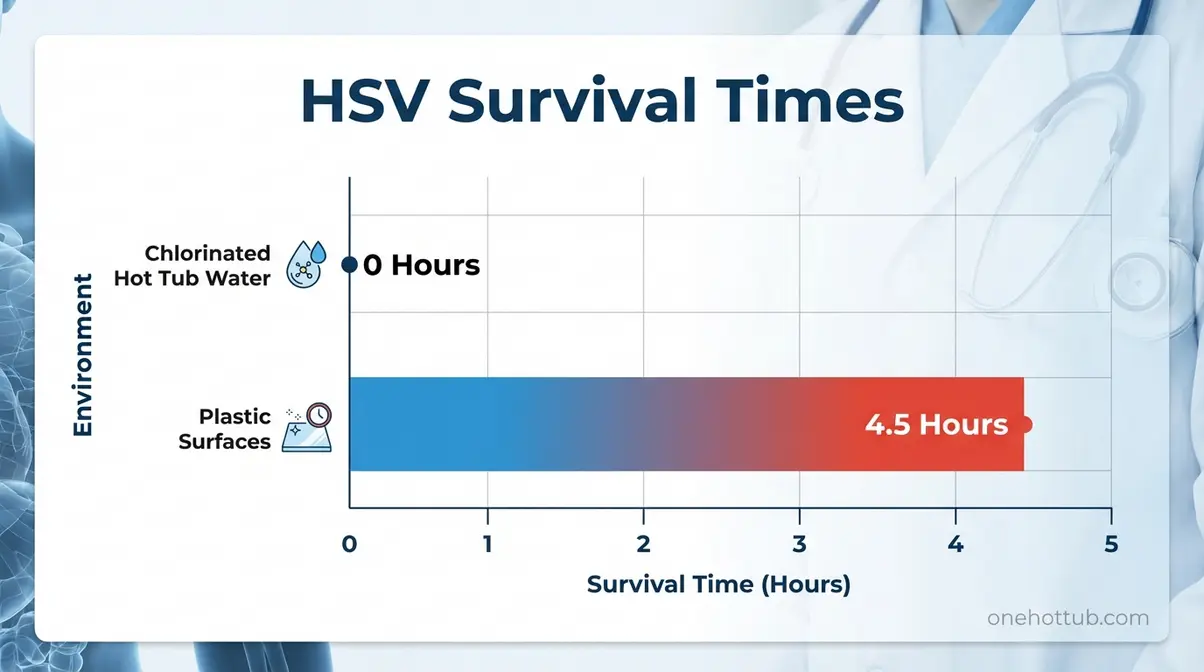
Caption: HSV survival drops to zero in properly chlorinated hot tub water — compare that to up to 4.5 hours on warm, humid plastic surfaces, where the virus lingers longest outside the body.
How Chemicals & Heat Destroy HSV
HSV is what virologists call an enveloped virus — meaning it’s wrapped in a fatty outer lipid membrane that the virus needs to infect cells. Chlorine and bromine (both halogens) attack and dissolve this envelope almost instantly, rendering HSV completely non-infectious before it can reach another person.
A peer-reviewed study published in a JAMA-affiliated journal (Nerurkar et al., 1983 — PMID 6315978) found that HSV was immediately inactivated in spa water containing standard halogen levels, with no viable virus recovered from actual health spa samples. On warm, humid plastic surfaces at hot tub temperatures, however, HSV survived up to 4.5 hours. While this is a 1983 study, modern medical consensus — including WHO guidance on herpes — consistently confirms that HSV-2 is transmitted through direct genital or skin contact, not through water.
Hot tub temperatures themselves add a second layer of protection. Standard hot tubs run at 100–104°F (38–40°C), and heat at this level accelerates the breakdown of viral proteins. A properly maintained hot tub with chlorine levels of 1–3 ppm or bromine at 3–5 ppm creates an environment where HSV cannot survive, let alone reach infectious concentrations. To learn more about how STDs behave in hot tub water, the chemistry is similarly decisive across other pathogens.
But what about bath water — where there’s no chlorine? And what if you have an active outbreak and want to soak? Both questions have clear answers.
Hot Tub Use During an Outbreak
If you have herpes and you’re wondering whether a soak is safe for you and others, your concern shows real consideration — and the answer is reassuring on the transmission side, with one personal caveat.
For other bathers, the risk remains zero. Water dilution combined with halogen inactivation means the viral load reaching another person is effectively nonexistent. Even bath water, which lacks chlorine, dilutes the virus so rapidly that transmission via shared bath water is not documented in medical literature.
For you, soaking during an active outbreak is a different calculation. Hot water and chemicals can irritate open sores, delay healing, and cause real discomfort. If you have active lesions, skipping the hot tub until they heal is sound self-care — not because you’ll infect others through the water, but because your own skin needs a break.
“If you have an active cold sore (HSV-1), soaking in a shared hot tub won’t spread it through the water — but avoid kissing or sharing drinks while sores are visible, as those routes do carry real risk.”
The Real Hot Tub Risk: Hot Tub Rash vs. Herpes
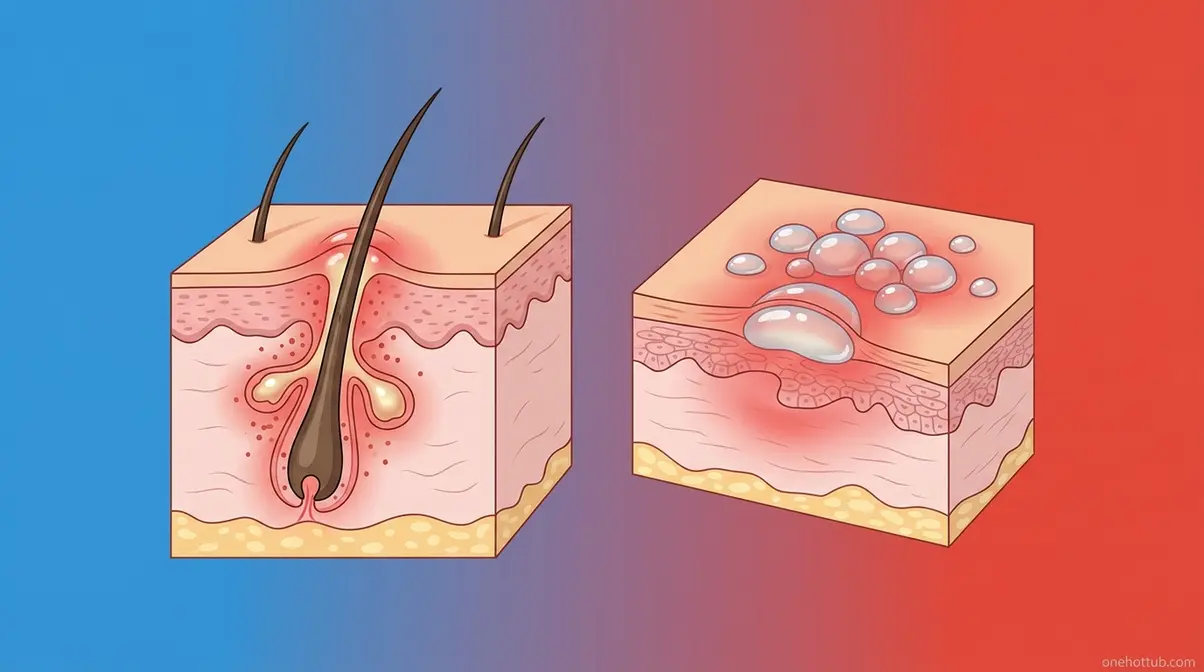
Here’s what hot tubs can give you — and it has nothing to do with herpes. The genuine risk is hot tub folliculitis, a skin infection caused by Pseudomonas aeruginosa, a bacterium that thrives in warm, poorly maintained water. It’s the most common hot tub health risk, and it’s frequently mistaken for a herpes outbreak.
Understanding this distinction matters. If you’ve developed a rash after a soak and are searching “can you get herpes from a hot tub,” the far more likely explanation is bacterial folliculitis — a treatable condition with a completely different cause, appearance, and course.
Folliculitis vs. Herpes Differences
Pseudomonas aeruginosa (the bacterium behind hot tub rash) causes itchy, red bumps centered on hair follicles, typically appearing 8 hours to 5 days after hot tub exposure. The rash concentrates in areas your swimsuit covered — trunk, buttocks, and upper arms. Some people also experience mild fever, fatigue, or earache alongside the skin symptoms (Cleveland Clinic, 2026).
Herpes, by contrast, presents as clustered blisters or ulcers on an inflamed base, often with a burning or tingling sensation — not generalized itchiness. Herpes lesions recur in the same location and are not follicle-centered.
The table below maps the key differences for quick reference:
| Feature | Hot Tub Folliculitis | Herpes (HSV) |
|---|---|---|
| Cause | Pseudomonas aeruginosa (bacteria) | Herpes simplex virus (HSV-1 or HSV-2) |
| Appearance | Red bumps, pustules around hair follicles | Clustered blisters or ulcers on red base |
| Primary sensation | Itchy | Burning, tingling, painful |
| Location | Swimsuit-covered areas (trunk, buttocks) | Oral, genital, or anal region |
| Onset after exposure | 8 hours – 5 days post-soak | Days to weeks after initial exposure |
| Recurrence pattern | After hot tub exposure only | Recurs at same site repeatedly |
| Systemic symptoms | Possible mild fever, fatigue | Possible fever during first outbreak |
| Resolution | 1–2 weeks, often without treatment | Managed with antiviral medication |
| Diagnosis | Clinical exam + bacterial culture | Viral PCR swab or clinical exam |
If you’re uncertain which condition you have, a clinician can distinguish them quickly — a swab or culture removes all guesswork.
5 Hygiene Steps for Hot Tub Safety
You can’t contract herpes from hot tub water, but you can reduce your risk of bacterial infections like folliculitis. Follow these five steps every time:
- Shower before and after entering. Rinsing before reduces contamination you bring into the water; showering after removes Pseudomonas bacteria before they can colonize hair follicles.
- Check the chemical levels. Ask staff or use test strips to confirm chlorine is 1–3 ppm or bromine is 3–5 ppm. Poorly maintained water is where bacterial risk rises sharply.
- Limit soak time. Extended exposure — particularly over 15–20 minutes — increases the time bacteria have to penetrate follicles. Take breaks and cool down periodically.
- Avoid the hot tub if you have open sores or broken skin. This protects you from bacterial entry, not herpes transmission. Open wounds are a direct route for Pseudomonas infection.
- Wash swimwear after each use. The Wisconsin Department of Health Services notes that Pseudomonas can persist in unwashed swimwear and cause repeated folliculitis exposure (WDHS, 2026).
Herpes From Toilet Seats or Towels?
“You cannot catch herpes from toilet seats, hot tubs, or any other casual contact.”
This widely cited medical position reflects a consistent finding across decades of virology research: HSV requires direct mucous membrane or skin-to-skin contact to transmit. Toilet seats, door handles, and shared surfaces simply don’t provide the conditions the virus needs, especially when proper hot tub surface cleaning protocols are followed.
The Transmission Hierarchy applies here too. Dry, cold surfaces sit just above water — near-zero risk, not absolute zero, but close enough that no documented case of toilet-seat herpes transmission exists in peer-reviewed literature.
Hard Surfaces vs. Damp Items
On dry surfaces like toilet seats, HSV degrades quickly. Research published in Pediatrics (Nerurkar et al., 1982 — PMID 6289234) found that HSV isolated from oral lesions survived up to two hours on skin, three hours on cloth, and four hours on plastic at room temperature — but critically, these survival times apply under humid, controlled laboratory conditions, not the dry environment of a typical toilet seat. In real-world conditions, survival is considerably shorter.
Damp shared items — wet towels, washcloths, or damp clothing — represent a slightly elevated theoretical risk compared to dry surfaces, because moisture extends survival time. However, even this risk is considered negligible by medical consensus, and no documented transmission via shared towels has been confirmed. The virus still requires direct contact with a mucous membrane or broken skin to establish infection — passive contact with a damp towel is not the same as direct skin-to-skin touch.
Does herpes survive on a surface in heat? Hot environments actually accelerate HSV degradation. High temperatures destabilize the viral envelope the same way hot tub water does, which is why outdoor surfaces in warm weather pose even less risk than cool, indoor ones.
Can You Get Herpes From Kissing or Sharing Items?

This is where The Transmission Hierarchy shifts. Move from surfaces to direct oral contact, and you move from negligible risk to genuine risk. The WHO reported in December 2024 that over 1 in 5 adults worldwide has a genital herpes infection — a figure that underscores how readily HSV transmits through the routes that actually matter: direct contact and saliva.
Sharing Drinks, Food, and Smokes
Sharing drinks, cigarettes, or joints with someone who has HSV-1 (oral herpes and cold sores) does carry a genuine, if low, transmission risk. The virus travels in saliva and on oral skin — and any item that moves from one person’s mouth to another’s creates a potential pathway.
The risk is meaningfully higher when the other person has an active cold sore or visible lesion. During an outbreak, viral shedding is at its peak, and the concentration of HSV in saliva rises significantly. Outside of active outbreaks, asymptomatic shedding still occurs — meaning someone can transmit HSV-1 without knowing they’re infectious, according to CDC guidance on herpes.
Sharing items is not the same as kissing — the virus concentration on a shared drink rim is lower than during direct oral contact — but the risk is real enough to warrant caution, particularly when sores are visible.
Kissing and HSV-1 vs. HSV-2
Kissing is one of the primary transmission routes for HSV-1 (the strain responsible for oral herpes and cold sores). Most HSV-1 infections are acquired during childhood through casual kissing with family members, which is why oral herpes is so prevalent globally.
HSV-2 (the strain most associated with genital herpes) is transmitted primarily through genital-to-genital or oral-to-genital contact during sexual activity. Kissing someone with HSV-2 on the genitals is a recognized — though less common — transmission route. Kissing someone with HSV-2 on the mouth is possible but rare, since HSV-2 doesn’t establish oral infections as readily as HSV-1.
The practical takeaway: if you’re kissing someone with a visible cold sore, transmission risk is real and present. If you’re kissing someone with genital HSV-2, mouth-to-mouth kissing carries very low risk — but open communication with your partner and consultation with a clinician is the right approach. Antiviral suppressive therapy, such as valacyclovir, has been shown to reduce HSV transmission risk between partners (ASHA Sexual Health, 2026).
Protecting Yourself and When to See a Doctor
You now have the full picture: hot tub water is safe, bacterial folliculitis is the real spa concern, dry surfaces carry negligible risk, and direct oral or sexual contact is where genuine HSV transmission occurs.
- See a doctor if:
- You develop clustered blisters, burning sores, or painful ulcers — especially in the genital, anal, or oral area — within days to weeks of a potential exposure
- You have a rash after hot tub use that doesn’t resolve within two weeks, or that’s accompanied by fever, fatigue, or ear pain (this suggests folliculitis requiring treatment)
- You’re in a relationship with a partner who has herpes and want to discuss suppressive antiviral therapy, safer sex strategies, or testing options
- You’re pregnant and concerned about HSV exposure — this is a situation requiring prompt medical attention
A clinician can distinguish herpes from folliculitis with a simple swab. Early antiviral treatment shortens outbreak duration and reduces the risk of transmission to partners. You don’t need to guess — a 10-minute appointment provides clarity that no online article can replace.
Frequently Asked Questions
Can herpes be passed through bath water?
Herpes cannot be transmitted through bath water, including shared bathtubs. HSV requires direct skin-to-skin or mucous membrane contact to infect a new host. Even in unchlorinated bath water, the virus dilutes rapidly and cannot reach infectious concentrations. A peer-reviewed study (Nerurkar et al., 1983) found no viable HSV in spa water samples. The risk from shared bath water is not documented in medical literature.
How long can herpes live in water?
HSV survives for essentially zero time in properly chlorinated hot tub water — standard halogen levels inactivate the virus almost immediately. In unchlorinated tap water, limited survival of a few hours has been observed in laboratory conditions, but infectious concentrations capable of causing transmission are not achievable in real-world water environments. The Public Health Agency of Canada confirms that standard disinfectants rapidly inactivate HSV.
Can herpes spread in a chlorinated pool?
No — herpes cannot spread in a chlorinated pool. The halogen disinfectants used in pools (chlorine at 1–3 ppm) destroy HSV’s lipid envelope almost instantly, rendering the virus non-infectious. The WHO confirms that HSV-2 spreads through direct genital or skin contact, not through water. Swimming with someone who has herpes — or swimming during your own outbreak — poses no transmission risk to other swimmers via the water itself.
Does Herpes Survive on Hot Surfaces?
Herpes survives poorly on surfaces, and heat accelerates its destruction. Under laboratory conditions, HSV can survive 2-4 hours on plastic or cloth at room temperature (Nerurkar et al., 1982). Heat degrades the virus’s fatty outer envelope — the same mechanism by which hot tub temperatures (100–104°F) contribute to inactivation. Outdoor surfaces in warm weather, and hot surfaces in general, offer even less survival time. No documented case of HSV transmission via a heat-exposed surface exists in medical literature.
Can you get herpes from a toilet seat?
No — you cannot get herpes from a toilet seat. HSV dies quickly on dry surfaces and requires direct mucous membrane or skin-to-skin contact to transmit. Toilet seats are dry, cool, and far removed from the mucosal tissue HSV needs to infect. Medical consensus, reflected in Hopkins Medicine’s herpes overview, is unambiguous: casual contact with inanimate objects does not transmit herpes.
The Bottom Line: Use the Right Framework
For anyone anxious and asking, can you get herpes from a hot tub, the science delivers a clear and consistent answer. The herpes simplex virus is inactivated almost immediately in properly maintained hot tub water — standard chlorine and bromine levels create an environment where HSV cannot survive. Over 1 in 5 adults worldwide carries genital herpes (WHO, December 2024), yet no documented case of hot tub water transmission exists, because the biology simply doesn’t support it.
The Transmission Hierarchy gives you a lasting mental model: water sits at zero risk, dry surfaces near-zero, shared saliva items carry low but real risk, and direct skin-to-skin contact is where transmission actually happens. Apply this framework to any future question about herpes and casual contact — it holds.
If you’ve developed a rash after a hot tub soak, the far more likely cause is bacterial folliculitis from Pseudomonas aeruginosa — treatable, common, and completely unrelated to herpes. And if you have a genuine concern about HSV exposure through kissing, sexual contact, or a partner’s diagnosis, a conversation with your doctor is the most productive next step. A clinician can test, advise on antiviral options, and help you and your partner navigate the situation with accurate information — not anxiety.



