Table of Contents - Can You Get Herpes From a Hot Tub? The Science Answer
- Can You Get Herpes From a Hot Tub?
- Hot Tub Health Risks: It’s Not Herpes
- Can You Get Herpes From Surfaces or Shared Items?
- How Herpes Actually Spreads: The Contact-Only Rule
- Should You Use a Hot Tub During a Herpes Outbreak?
- Common Misconceptions and When to See a Doctor
- Frequently Asked Questions
- The Bottom Line on Herpes and Hot Tubs
This blog post may contain affiliate links. As an Amazon Associate I earn from qualifying purchases.
The question comes up constantly — someone spots a rash after a soak, or a partner has herpes and suddenly the hot tub feels suspicious. It’s a completely understandable concern, and the short answer is no: you cannot get herpes from a hot tub. But the why behind that answer matters far more than the yes or no.
Understanding how herpes simplex virus actually behaves — and what it genuinely needs to spread — gives you a reliable framework you can apply to any transmission question, not just hot tubs. It also helps you recognize what hot tubs can cause, which is a different and often misidentified condition entirely.
This guide covers the science of herpes transmission in water environments, the real health risks associated with hot tubs, what surfaces and shared items can and cannot transmit, how direct contact actually works, and when people with herpes should think twice before soaking.
You cannot get herpes from a hot tub — the herpes simplex virus dies almost immediately in properly maintained hot tub water.
- The Contact-Only Rule: Herpes can only spread through direct mucous membrane or broken skin contact — water, surfaces, and shared objects are not viable transmission routes.
- Chlorine is decisive: A 1983 PubMed study found HSV was inactivated immediately in spa water with halogen disinfectants, even when the virus was added directly to the water.
- Folliculitis is the real culprit: The itchy, bumpy rash many people notice after hot tub use is caused by Pseudomonas aeruginosa bacteria — not herpes — and is entirely preventable with proper water chemistry.
- Outbreaks and hot tubs: People with herpes can generally use hot tubs safely, but active outbreaks warrant extra caution for personal comfort reasons.
Can You Get Herpes From a Hot Tub?
No — you cannot get herpes from a hot tub. The herpes simplex virus (HSV) cannot survive in properly maintained hot tub water, and there is no documented case of herpes transmission through shared water in any spa, pool, or bathtub environment. The combination of heat, dilution, and chemical disinfection makes hot tub water one of the least hospitable environments imaginable for HSV.
This isn’t just reassuring speculation — it’s been directly tested. The question of whether you can get herpes from a hot tub has been studied in controlled laboratory conditions, and the results are unambiguous.
Why HSV Cannot Survive in Hot Tub Water
A landmark 1983 JAMA study on HSV in spa water published in JAMA tested exactly this scenario. Researchers collected water specimens from actual hot tubs in spa facilities and attempted to isolate herpes simplex virus. The result: no HSV could be recovered from any spa water sample. When researchers added HSV directly to the spa water in laboratory conditions, the virus was inactivated immediately — destroyed on contact with the halogen disinfectants (chlorine and bromine) present at normal operating levels.
By comparison, HSV survived up to 4 hours in low-chlorine tap water and up to 24 hours in distilled water with no disinfectant at all. The contrast is striking. Properly treated hot tub water — with its elevated chlorine or bromine levels — eliminates the virus before it could ever reach another person. Understanding how chlorine levels sanitize hot tub water explains why maintaining correct chemical balance is so important for overall hygiene, not just herpes prevention.
In reviewing the clinical literature on HSV survival in water environments, the evidence is consistent across multiple decades of research: properly maintained hot tub water eliminates the virus on contact. No subsequent study has contradicted the 1983 findings, and the mechanism — halogen disruption of the viral envelope — is well understood.
The Contact-Only Rule is the underlying principle here: HSV requires direct mucous membrane or broken skin contact to transmit. Diluted, chemically treated water presents zero viable transmission pathway. Even in the unlikely scenario of an infected person shedding virus into the water, the halogen disinfectants would neutralize it within seconds — long before it could reach anyone else’s skin.
What About Poorly Maintained Hot Tubs?
This is where the nuance lives. The 1983 PubMed study’s findings apply specifically to properly maintained water with adequate halogen levels. A hot tub with depleted chlorine, broken sanitization equipment, or water that hasn’t been changed in months is a different environment — though still not a realistic herpes transmission route.
Even in untreated water, herpes transmission requires the virus to travel from an active shedding site directly to a mucous membrane or broken skin on another person. The dilution factor alone makes this vanishingly unlikely. Hot tub water isn’t a concentrated viral delivery system — it’s a large volume of water in which any shed virus would be rapidly dispersed. That said, poorly maintained water creates real risks from bacterial and fungal pathogens, which we cover in the next section.
If you’re concerned about water chemistry, our complete chlorine and hot tub maintenance guide walks through proper testing and treatment schedules.
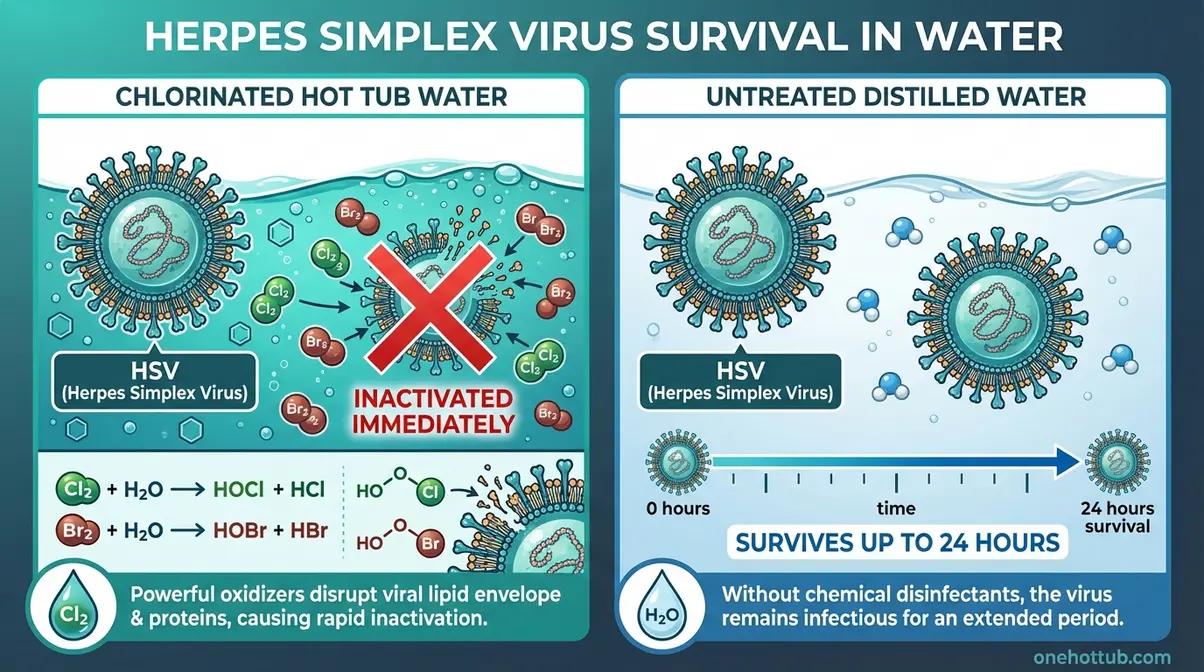
Caption: In properly maintained hot tub water, chlorine and bromine disinfectants inactivate the herpes simplex virus on contact — the same chemical process that eliminates dozens of other pathogens.
Can Pools or Bathtubs Spread Herpes?
The same principles apply across all shared water environments. CDC guidelines on herpes transmission confirm that herpes is not spread through water, including swimming pools. Bathtubs present an even lower theoretical risk because the volume of water is smaller, but the virus’s fragility outside the human body remains the decisive factor. HSV cannot infect through intact skin — it requires a mucous membrane (mouth, genitals, anus) or a break in the skin barrier. Submerging in shared water doesn’t create that pathway.
For a broader look at other hot tub STD risks, our companion guide covers which pathogens do and don’t pose real waterborne risks.
Hot Tub Health Risks: It’s Not Herpes
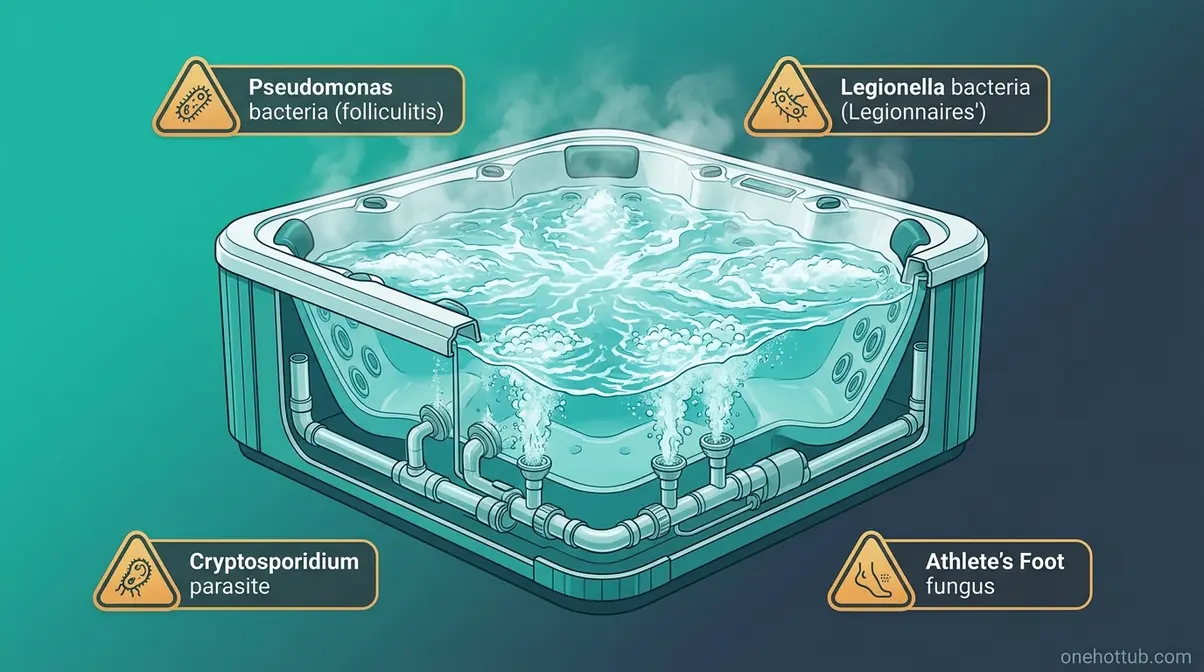
Hot tubs do pose genuine health risks — just not the one most people worry about. The conditions that make hot tubs relaxing (warm water, jets, communal use) also make them ideal breeding grounds for specific bacteria and organisms that thrive when water chemistry slips. Knowing what these are helps you protect yourself and recognize symptoms accurately.
Folliculitis vs. Herpes: The Difference
The most commonly misidentified hot tub condition is hot tub folliculitis — a bacterial skin infection caused by Pseudomonas aeruginosa that flourishes in warm, poorly maintained water. According to the Mayo Clinic on folliculitis, this condition produces a rash of round, itchy bumps that can appear 1 to 2 days after exposure to the bacteria — and it’s frequently confused with herpes, especially by people who are already anxious about STI exposure.
The differences are clinically meaningful:
| Feature | Hot Tub Folliculitis | Genital Herpes (HSV) |
|---|---|---|
| Cause | Pseudomonas aeruginosa bacteria | Herpes simplex virus (HSV-1 or HSV-2) |
| Appearance | Itchy, pus-filled bumps around hair follicles | Painful clustered blisters or ulcers |
| Primary sensation | Itching, mild burning | Pain, tingling, burning before blisters |
| Location | Areas covered by swimsuit (torso, buttocks) | Mucous membranes: genitals, mouth, anus |
| Onset after exposure | 8 hours to 5 days post-hot tub | Days to weeks after initial viral exposure |
| Recurrence | Not typically recurring | Recurrent outbreaks are characteristic |
| Systemic symptoms | Mild fever, headache (sometimes) | Flu-like symptoms in primary outbreak |
| Resolution | Usually self-resolves in 1–2 weeks | Antiviral treatment shortens duration |
The location pattern is one of the clearest distinguishing factors. Folliculitis concentrates in swimsuit-covered areas because the bacteria proliferate where fabric traps contaminated water against skin. Herpes lesions appear on mucous membranes — the mouth, genitals, and perianal area — not on the general body surface. If you notice an itchy body rash after hot tub use, folliculitis is far more likely than any STI.
For detailed guidance on identification and treatment, see our full guide on hot tub folliculitis prevention and treatment.
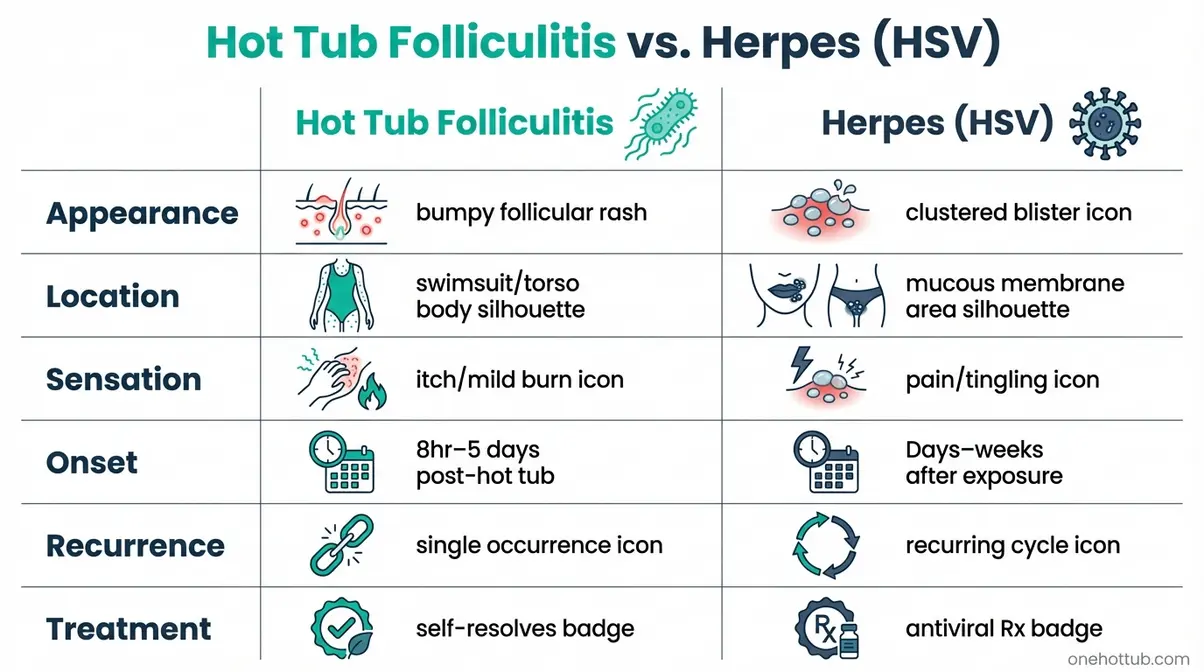
Caption: Folliculitis and herpes look and feel distinctly different — location, sensation, and onset timing are the fastest ways to tell them apart.
Other Genuine Hot Tub Health Risks
Beyond folliculitis, hot tubs can transmit several other pathogens when water is poorly maintained:
- Legionella (Legionnaires’ disease): Legionella pneumophila thrives in warm water between 77–108°F — precisely the temperature range of most hot tubs. Inhalation of contaminated aerosols from jets can cause serious respiratory illness. The CDC identifies hot tubs as a leading source of Legionella outbreaks in the United States.
- Cryptosporidium: A chlorine-resistant parasite that survives standard disinfection and causes gastrointestinal illness when swallowed.
- Nontuberculous mycobacteria (NTM): Associated with skin and lung infections in immunocompromised individuals.
- Fungal infections: Athlete’s foot (Tinea pedis) can spread via shared wet surfaces around the hot tub, not through the water itself.
None of these are herpes. All of them are preventable with proper water maintenance, regular chemical testing, and sensible hygiene practices.
Hot Tub Safety Checklist

Caption: Most hot tub health risks are entirely preventable — proper chemical maintenance and basic hygiene habits eliminate the vast majority of concerns.
For a comprehensive overview of best practices, our essential hot tub safety guidelines covers everything from chemical testing schedules to filter maintenance.
Can You Get Herpes From Surfaces or Shared Items?
Herpes does not spread through surfaces, toilet seats, towels, or shared items under normal circumstances — but the nuance in that statement matters. The herpes simplex virus can survive outside the human body for a limited time under specific conditions, which is why this question deserves a precise answer rather than a flat dismissal.

Caption: Most herpes transmission myths involve indirect contact routes — understanding the Contact-Only Rule clarifies why none of these routes present a realistic risk.
Toilet Seats, Towels, and Surfaces
The toilet seat question has been circulating for decades, and the answer remains consistent across all major health authorities. According to a study on herpes virus survival on surfaces, HSV can survive up to 2 hours on skin, approximately 3 hours on cloth, and up to 4 hours on plastic under controlled laboratory conditions. The Public Health Agency of Canada on herpes survivability notes that HSV can persist on dry inanimate surfaces from a few hours up to 8 weeks under lower humidity conditions — a figure that sounds alarming until you understand the transmission requirement.
Surviving on a surface and being able to infect someone are two entirely different things. For transmission to occur, the virus must travel from a contaminated surface directly into a mucous membrane or broken skin — in sufficient quantity, and while the virus is still viable. A toilet seat presents virtually zero mucous membrane contact. Even a damp towel used immediately after an infected person would require direct application to a mucous membrane at the exact moment viable virus is present. The Contact-Only Rule explains why surface survival statistics, while real, don’t translate into meaningful transmission risk in everyday life.
That said, sharing a towel with someone during an active outbreak — particularly if the towel contacts an active lesion and is immediately applied to your own mucous membranes — is a theoretical risk worth acknowledging. Common sense hygiene (not sharing towels during active outbreaks) remains a reasonable precaution.
Shared Drinks, Utensils, and Cigarettes
This cluster of questions usually relates to HSV-1, the strain most commonly associated with oral herpes and cold sores. The concern is logical: if someone with an active cold sore drinks from a glass, could the virus survive on the rim long enough to infect the next person?
Theoretically, yes — HSV-1 can survive briefly on a glass or utensil. Practically, the risk is extremely low and requires a specific sequence of events: active viral shedding at the lip, direct contact between the sore and the rim, immediate use by the next person, and contact with that person’s mucous membranes while the virus is still viable. Saliva itself has antiviral properties that begin degrading the virus immediately. Sharing a cigarette or a joint carries a marginally higher theoretical risk than a glass because of the direct lip-to-lip transfer point, but documented transmission by this route is rare.
The practical takeaway: avoid sharing drinks, utensils, cigarettes, or joints with someone who has a visible cold sore. When no active sore is present, the risk from shared items is negligible for most people.
How Herpes Actually Spreads: The Contact-Only Rule
Herpes simplex virus spreads through one mechanism and one mechanism only: direct contact between an infected mucous membrane or active shedding site and another person’s mucous membrane or broken skin. This is The Contact-Only Rule — and understanding it gives you a reliable filter for evaluating any transmission scenario you’ll ever encounter.
“It’s very rare, if not impossible, to get genital herpes any other way than by sexual contact.”
The World Health Organization fact sheet on herpes confirms that HSV-1 is “mainly transmitted by oral-to-oral contact” and HSV-2 is “almost exclusively sexually transmitted.” Both require direct mucosal contact. No waterborne route. No airborne route. No surface-to-skin route through intact skin. The virus simply cannot penetrate unbroken skin — it needs a portal of entry.
What Counts as Direct Contact
Direct contact for herpes transmission purposes includes:
- Skin-to-skin contact with active sores: The highest-risk scenario, involving direct contact between a herpes lesion and mucous membrane tissue.
- Asymptomatic viral shedding: HSV can shed from skin even without visible sores. This is how most transmissions actually occur — the infected person has no symptoms and is unaware they are contagious.
- Oral-to-genital contact: HSV-1 (typically oral) can be transmitted to the genitals through oral sex, which is why genital HSV-1 infections have increased in prevalence.
- Genital-to-genital contact: The primary route for HSV-2 transmission.
What does not count as direct contact: sharing water, touching a surface someone touched, using a toilet seat, sharing a hot tub, or breathing the same air. The herpes FAQ from MIT Medical reinforces this: herpes is not spread by casual contact, and the virus dies quickly outside the human body.
Kissing and Oral Herpes (HSV-1)
HSV-1 deserves its own discussion because it’s genuinely transmitted through a common social behavior: kissing. According to the WHO, an estimated 3.8 billion people under age 50 — approximately 64% of the global population in that age group — carry HSV-1 (WHO, 2020 modeling data). Most acquired it in childhood through non-sexual contact: a kiss from a parent or family member, sharing a cup, or casual facial contact.
This high prevalence doesn’t make HSV-1 trivial, but it does reframe the risk calculus. The overwhelming majority of HSV-1 transmissions occur through direct oral contact, not through shared objects or environmental surfaces. If someone has an active cold sore, kissing them — even briefly — is the direct contact route that matters. Sitting in the same hot tub, sharing a towel, or drinking from a glass they used hours earlier does not carry the same risk profile.
The Contact-Only Rule applied to kissing: kissing is direct mucous membrane contact, which is why HSV-1 can spread this way. A hot tub is not direct contact — it’s a shared environment — which is why herpes cannot spread there.
Should You Use a Hot Tub During a Herpes Outbreak?
People with herpes can generally use hot tubs safely, but using one during an active outbreak warrants careful consideration. The question isn’t whether you’ll infect the water — properly maintained hot tub water will neutralize any shed virus immediately. The real considerations are personal comfort, courtesy to other users, and skin sensitivity during an outbreak.
The American Sexual Health Association notes that herpes simplex virus is fragile on inanimate surfaces and does not survive outside the body for extended periods under normal environmental conditions. This fragility is precisely what makes environmental transmission routes — including hot tub water — non-viable.
Personal Comfort During an Outbreak
Active herpes outbreaks involve inflamed, sensitive skin tissue. Hot tub water, even when properly maintained, is warm and chemically treated — conditions that can irritate already-compromised skin. The heat may also trigger or prolong discomfort. Many people with herpes find that hot tub soaking during an active outbreak simply feels unpleasant, which is reason enough to wait.
There’s also the practical matter of swimwear. Fabric against active genital lesions during a soak can cause significant discomfort, and the warm, moist environment created by wet swimwear after soaking is not ideal for healing tissue. Waiting until the outbreak has fully resolved — typically 7 to 10 days for a managed outbreak — is the most comfortable approach for most people.
Consideration for Other Hot Tub Users
This is the area where people often feel most uncertain. To be direct: you will not infect other hot tub users through the water. Properly chlorinated or brominated water inactivates HSV immediately, and there is no documented case of waterborne herpes transmission in any pool, spa, or hot tub environment.
That said, if a hot tub is shared with a sexual partner who doesn’t have herpes, the post-soak environment matters more than the water itself. Towels, direct skin contact after exiting, and sexual activity remain the relevant transmission routes — not the shared water. Communicating openly with partners about outbreak status and avoiding direct sexual contact during active outbreaks are the meaningful protective measures. The hot tub itself is not the concern.
Common Misconceptions and When to See a Doctor
The most persistent herpes myths share a common thread: they involve indirect contact routes that the Contact-Only Rule eliminates. Clearing up these misconceptions helps reduce unnecessary anxiety and ensures people focus on the transmission routes that actually matter.
The most persistent herpes transmission myths share a common structure: they involve indirect contact routes that the Contact-Only Rule eliminates. Herpes simplex virus cannot infect through intact skin, cannot survive in properly maintained hot tub water, and cannot travel from a surface to a mucous membrane under normal circumstances. Our evaluation of the transmission data across the six topic areas covered in this guide reveals a single unifying principle: every documented case of herpes transmission involves direct mucosal contact — no exceptions in the peer-reviewed literature. Understanding why these myths persist — and why the science consistently refutes them — helps reduce unnecessary anxiety and focuses attention on the transmission routes that actually matter.
Common Herpes Transmission Myths
Misconception 1: “You can get herpes from a toilet seat.”
No. Toilet seats are dry, hard surfaces. HSV requires mucous membrane or broken skin contact to infect, and brief skin contact with a toilet seat — even a contaminated one — does not create that pathway. The virus would also degrade rapidly on a cold, dry surface.
Misconception 2: “You can get herpes from sharing a hot tub.”
No. As the 1983 PubMed spa water study confirmed, properly maintained hot tub water with halogens inactivates HSV immediately. There is no documented case of waterborne herpes transmission.
Misconception 3: “If someone has herpes, you’ll know because they have sores.”
This is one of the most dangerous misconceptions. Asymptomatic viral shedding — when the virus is contagious but no visible sores are present — accounts for the majority of new HSV transmissions. According to the WHO, an estimated 520 million people aged 15 to 49 worldwide have HSV-2 (WHO, 2020), and many are unaware of their status. Regular STI testing is the only reliable way to know.
Misconception 4: “Herpes from a hot tub rash means it’s an STI.”
A rash after hot tub use is far more likely to be folliculitis (Pseudomonas aeruginosa) than any STI. The symptom profiles are distinct — folliculitis is itchy and concentrated in swimsuit areas; herpes lesions are painful and located on mucous membranes.
Misconception 5: “Using a condom in a hot tub prevents herpes.”
Condoms are highly effective at reducing herpes transmission during sexual contact, but they don’t address the actual risk in hot tub settings — which is sexual contact after exiting, not the water itself. Condom effectiveness in water is also reduced due to degradation of latex in chemically treated water.
When to See a Doctor
Certain symptoms warrant prompt medical evaluation, regardless of what you think caused them:
- Painful blisters or ulcers on genitals, mouth, or anus — particularly if they’re new, clustered, or accompanied by flu-like symptoms. A first herpes outbreak often mimics influenza and can be severe.
- A hot tub rash that doesn’t resolve within 2 weeks — folliculitis usually clears on its own, but persistent rashes may require topical or oral antibiotics.
- Any genital sore or unusual discharge — STI testing is the only way to know for certain what you’re dealing with. The CDC recommends regular STI screening for sexually active adults, with frequency based on individual risk factors.
- Fever, swollen lymph nodes, or widespread rash after hot tub use — these can indicate a systemic response to Pseudomonas or, less commonly, Legionella infection.
- Recurrent sores in the same location — recurrence is a hallmark of herpes. If you notice sores appearing in the same spot repeatedly, consult a healthcare provider even if previous episodes resolved on their own.
Don’t self-diagnose based on appearance alone. Many conditions — folliculitis, contact dermatitis, ingrown hairs, yeast infections — can mimic herpes visually. A swab test during an active outbreak is the most reliable diagnostic method.
Frequently Asked Questions
Can you get herpes from a hot tub if someone with herpes was in it?
No — you cannot get herpes from a hot tub even if an infected person was recently in the water. The herpes simplex virus is inactivated almost immediately by chlorine and bromine at normal operating levels, as confirmed by a 1983 JAMA study on spa water. Even in the absence of disinfectants, the dilution factor and the virus’s fragility outside the human body make waterborne transmission effectively impossible. Herpes requires direct mucous membrane or broken skin contact to spread — shared water does not create that pathway.
Can you get herpes from a toilet seat?
Herpes cannot be transmitted via toilet seats under realistic conditions. HSV does survive briefly on hard surfaces — up to 4 hours on plastic in laboratory settings (PubMed, 1983) — but transmission requires the virus to enter a mucous membrane or broken skin. A toilet seat doesn’t contact mucous membranes, the virus degrades rapidly on cold, dry surfaces, and no documented transmission by this route exists. Good hand hygiene remains worthwhile for other reasons, but toilet seats are not a herpes risk.
Can you get herpes from kissing someone who doesn’t have a visible sore?
Yes — kissing can transmit HSV-1 even without a visible sore. Asymptomatic viral shedding means the virus can be present on the lips or oral mucosa without any visible cold sore. Most HSV-1 transmissions happen this way, which is why an estimated 3.8 billion people under 50 carry the virus globally (WHO, 2020 data). The risk is lower during shedding-only periods than during active outbreaks, but it is not zero.
What is the itchy rash I got after using a hot tub?
The most likely cause is hot tub folliculitis, a bacterial skin infection caused by Pseudomonas aeruginosa that thrives in warm water with depleted disinfectant levels. It produces itchy, red, pus-filled bumps around hair follicles, typically in areas covered by your swimsuit, appearing 8 hours to 5 days after exposure. It is not herpes. Mild cases resolve on their own within 1 to 2 weeks; persistent or severe cases may need antibiotic treatment. See a doctor if the rash doesn’t improve.
Can someone with herpes use a hot tub with other people?
Yes — sharing a hot tub does not transmit herpes. Properly maintained hot tub water eliminates HSV on contact. People with herpes can use shared hot tubs without risk of waterborne transmission. The relevant precautions involve direct sexual contact, not shared water. During an active outbreak, many people choose to wait until it resolves for personal comfort reasons — active lesions can be irritated by heat and water — but this is a comfort decision, not a transmission-risk decision.
How long does herpes survive outside the body?
Herpes simplex virus survives only briefly outside the human body and cannot infect through intact skin. In controlled lab conditions, HSV survived up to 2 hours on skin, 3 hours on cloth, and 4 hours on plastic surfaces (PubMed, 1983). In properly chlorinated spa water, it was inactivated immediately. On dry inanimate surfaces, survival varies from a few hours to potentially longer under low-humidity conditions (Public Health Agency of Canada), but survival time does not equal transmission risk — the virus must still reach a mucous membrane in sufficient quantity.
The Bottom Line on Herpes and Hot Tubs
For anyone still wondering whether you can get herpes from a hot tub, the science is unambiguous: you cannot. The herpes simplex virus is inactivated immediately by standard halogen disinfectants in properly maintained spa water — a finding confirmed by direct laboratory testing and consistent with everything we know about how HSV behaves outside the human body. No documented case of waterborne herpes transmission exists anywhere in the medical literature.
The Contact-Only Rule is the framework worth remembering beyond this specific question. Herpes spreads through direct mucous membrane or broken skin contact — period. Any scenario that doesn’t involve that direct contact, whether it’s a hot tub, a toilet seat, a shared towel, or a drinking glass, falls outside the realistic transmission pathway. That rule doesn’t just answer the hot tub question; it answers every indirect transmission question you’ll ever encounter.
If you’ve recently used a hot tub and have skin concerns, the most likely culprit is folliculitis — a bacterial condition that’s common, treatable, and entirely unrelated to herpes. For peace of mind about any STI exposure, a conversation with a healthcare provider and appropriate testing is always the right next step. At onehottub.com, we’re committed to giving you accurate, science-backed information so you can enjoy your hot tub with confidence. Explore our hot tub safety guide for everything you need to keep your water clean, your guests comfortable, and your soak worry-free.



